The NZSCM Diploma in Cosmetic Medicine

The NZSCM Diploma in Cosmetic Medicine is a structured,postgraduate pathway for vocationally registered doctors. It is the only New Zealand training that recognised with Medical Council of New Zealand and is delivered by NZSCM’s Education Faculty with a strong emphasis on patient safety, clinical judgement, and professional standards. Teaching combines formal workshops, supervised clinical work, peer learning, and summative assessment. Trainees are expected to progress to safe, independent practice across core cosmetic medicine modalities by graduation.
Training is undertaken across two academic years from February to February. Expect to commit around eight hours each week for reading, case preparation, peer group activity, and treating practice patients in order to meet logbook requirements. Workshops are compulsory and are delivered in Auckland on two full days across weekends through the year, typically running from 8.30 am to 4.30 pm. Each workshop blends lecture teaching with patient-based practical sessions in a cosmetic medical clinic environment so that knowledge and technical skill develop in parallel.
Across years one and two you will study head and neck anatomy in depth, the physiology of appearance and ageing, consultation and consent, and the science and technique of core modalities. Practical teaching covers botulinum toxins, hyaluronic acid fillers, dermal remodelling techniques such as needling, platelet-rich plasma and peels, radiofrequency ablation, and an introduction to energy-based devices with progression into threads, skin boosters and deoxycholic acid. The programme design emphasises complication recognition, avoidance, and management, cultural safety in consultation, and the medico-legal standards required for ethical practice.
Workshops are the engine room of the programme. Trainees rotate through lectures, case planning, and supervised injecting on patients, with observation and short assessments throughout. This format allows facilitators to identify strengths and gaps in real time and to target support appropriately. Industry partners contribute selected sessions so trainees gain balanced product knowledge and familiarity with device platforms while maintaining an evidence-based focus.
The academic year begins with a foundation weekend that orients new trainees to the curriculum, clinical photography, and building logs and practice processes, while second-year trainees undergo an early practical review of facial filler planning and technique. Subsequent weekends step through botulinum toxin, filler, invasive dermal remodelling, energy-based devices, skin and skin boosters, complications and threads, with integrated anatomy and risk-zone teaching. Teaching venues are St Cuthberts and Clinic 42 in Epsom, Auckland, which supports seamless movement from lectures to patient sessions
Year one builds core knowledge and safe technique in botulinum toxin and hyaluronic acid fillers, introduces dermal remodelling, and sets up your consultation, documentation and ethical practice. Year Two advances case complexity and breadth of modalities and tightens complication management. The first weekend of year two includes a structured practical assessment using a single-syringe scenario to stress clinical reasoning, treatment planning, and technical execution so trainers and facilitators can tailor support for the remainder of the year.
Assessment is continuous and summative. Every workshop includes a written and observed assessment of core knowledge, modality-specific skill, professionalism, ethics, cultural competence, and medico-legal understanding. Formal examinations comprise a one-hour multiple-choice exam with a 70 percent pass mark, and an Objective Structured Clinical Examination at the end of each academic year to test applied clinical decision-making and procedural skill in standardised stations. Each trainee must attend and present a presentation in their second year.
You will maintain procedural logbooks using the NZSCM online template. Botulinum toxin and hyaluronic acid fillers are compulsory modalities, and you must choose one additional modality from radiofrequency ablation, energy-based devices, or dermal remodelling. Minimum experience requirements include 50 botulinum toxin cases and 50 hyaluronic acid filler cases within the first 24 months of training. Logs must be updated monthly to support monitoring and feedback, and the practice visit is the definitive assessment of your applied clinical competence.
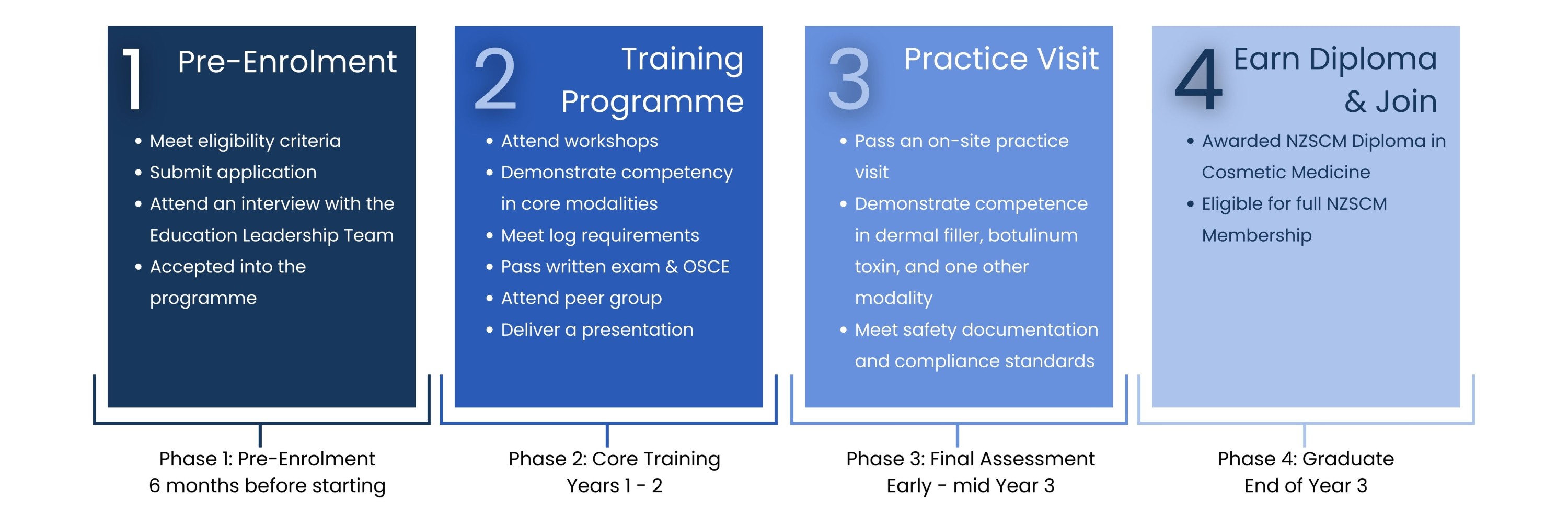
The NZSCM Diploma in Cosmetic Medicine is taught over two years, with structured workshops, lectures, examinations, and supervised clinical training. In the third year, trainees complete their logbooks and undergo a practice visit assessment. The final step before graduation.
Graduation is formally recognised at the NZSCM Annual Conference each year, where we celebrate this significant achievement and mark an important milestone in your cosmetic medicine journey.
Clinical supervision and collegial oversight are provided by the NZSCM Education Faculty for enrolled trainees and are limited to modalities taught within the programme. Supervision begins only after you have attended the relevant workshop. It does not extend to issuing Standing Orders to nurses. Trainees are advised not to purchase or administer a brand until training in that product has been undertaken within the programme.
Progress is supported by compulsory peer group meetings during both years, attendance at the Annual Scientific Meeting, and a culture of open discussion and shared learning at each workshop. Participation in the programme earns 150 CME credits per year, reflecting the breadth of activity and study required for safe, competent practice.
Plan for approximately eight hours per week for reading, online lectures, case write-ups, and treating practice patients. Workshops provide concentrated teaching and supervised experience, but consistent clinic time is essential to reach logbook thresholds and to embed safe technique and judgement. Expect regular feedback from facilitators, and expect to practise under supervision in line with Medical Council expectations until graduation.